Gluten directly affects gut health by triggering the release of zonulin, a protein that opens the tight junctions between cells in your intestinal lining. In people with celiac disease or non-celiac gluten sensitivity, this increased intestinal permeability allows partially digested food particles and bacteria to cross into the bloodstream, activating an immune response. The connection between gluten and gut health is well-studied, clinically documented, and — most importantly — manageable with the right approach.
As a registered nurse and a mom managing a fully gluten-free household, I’ve spent years translating the science of gut health into practical strategies that actually work in real life. This guide walks you through exactly what happens in your gut when you eat gluten, how to recognize damage, and the evidence-based steps to heal and thrive on a gluten-free diet.
What Happens in Your Gut When You Eat Gluten
When you eat foods containing wheat, barley, or rye, your digestive system breaks down the gluten protein into smaller fragments called gliadin peptides. Most proteins get fully digested, but gliadin is unusually resistant to human digestive enzymes. These partially digested fragments are where the trouble starts.
In sensitive individuals, gliadin triggers cells in the small intestine to release a protein called zonulin. Research led by Dr. Alessio Fasano at Massachusetts General Hospital identified zonulin as the key regulator of intestinal permeability. Zonulin acts like a signal that tells the tight junctions between your gut lining cells to open up — think of it as unlocking the gates in a fence that’s supposed to keep things out.
These tight junctions are the connections between the cells lining your small intestine. Normally, they form a selective barrier — letting nutrients through while keeping bacteria, toxins, and undigested food particles out. When zonulin forces them open, the barrier becomes “leaky,” allowing substances to pass into the bloodstream that shouldn’t be there.
What happens next depends on whether you have celiac disease or non-celiac gluten sensitivity:
- Celiac disease — Your immune system launches a full autoimmune attack. It produces antibodies (tissue transglutaminase antibodies, or tTG-IgA) that target and destroy the villi lining your small intestine. This is a systemic, progressive condition that causes measurable intestinal damage visible on biopsy.
- Non-celiac gluten sensitivity (NCGS) — Your body mounts an innate immune response without producing the autoimmune antibodies seen in celiac disease. You experience real symptoms — bloating, fatigue, brain fog, digestive distress — but without the villous atrophy that defines celiac. Research published by the Celiac Disease Foundation estimates NCGS may affect up to 6% of the U.S. population.
In both cases, the result is inflammation, impaired nutrient absorption, and a cascade of symptoms that can extend far beyond your digestive tract. Understanding this mechanism is the first step toward taking control of your gut health.
Understanding Your Gut: A Quick Anatomy Primer
Your gastrointestinal tract is a 30-foot system designed to break down food, absorb nutrients, and keep harmful substances out. The star of this story is the small intestine — about 20 feet of highly specialized tissue where roughly 90% of nutrient absorption happens.
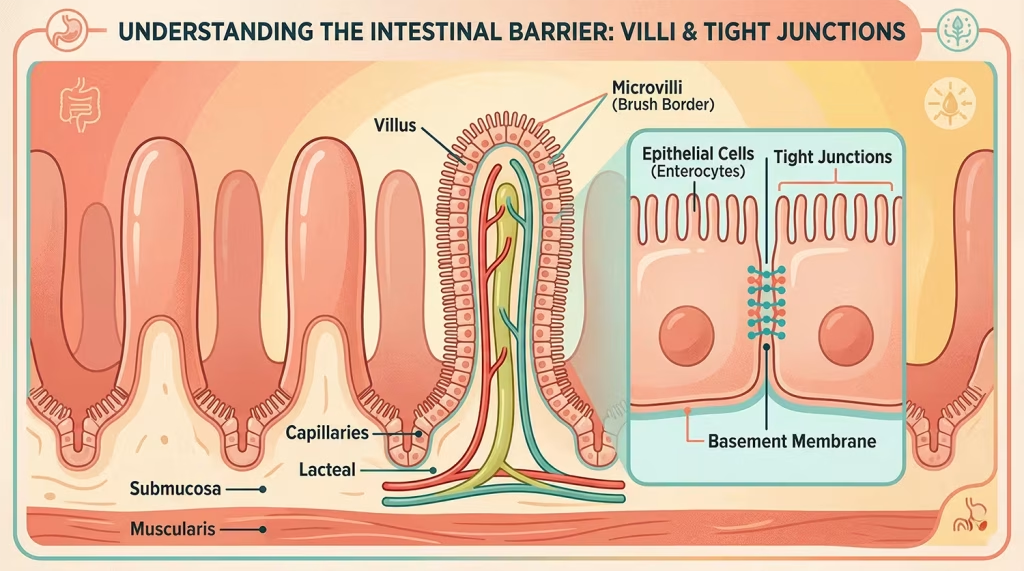
The inner walls of your small intestine are covered in millions of tiny, finger-like projections called villi. Each villus is covered in even tinier projections called microvilli. Together, they create an enormous surface area — roughly the size of a tennis court — that maximizes your body’s ability to absorb nutrients from food. When celiac disease destroys these villi (a process called villous atrophy), that surface area shrinks dramatically, and nutrient absorption plummets.
Here’s the part that surprises most people: the barrier between your gut contents and your bloodstream is just one cell thick. A single layer of epithelial cells, held together by those tight junctions we talked about, is all that separates the food passing through your intestine from your internal organs and immune system. It’s an incredibly thin line of defense — and it’s exactly what gluten compromises in sensitive individuals.
Living alongside those epithelial cells are trillions of microorganisms — bacteria, fungi, and viruses — collectively known as your gut microbiome. These organisms aren’t just passengers. They help digest certain fibers, produce essential vitamins (like vitamin K and some B vitamins), train your immune system, and communicate with your brain via the gut-brain axis. Research increasingly shows that the balance of your microbiome directly influences how your gut responds to gluten and how quickly it can heal after damage.
Signs Your Gut May Be Damaged by Gluten
Gut damage from gluten doesn’t always announce itself with obvious digestive symptoms. Many people with celiac disease or gluten sensitivity experience a wide range of symptoms that seem unrelated to digestion — which is why the average celiac diagnosis takes 6–10 years, according to Beyond Celiac.
Common Signs of Gut Damage from Gluten
- Persistent bloating, especially after meals containing grains
- Chronic diarrhea, constipation, or alternating between both
- Abdominal pain or cramping that doesn’t resolve
- Unexplained fatigue that sleep doesn’t fix
- Brain fog — difficulty concentrating, mental “fuzziness”
- Skin rashes, particularly dermatitis herpetiformis (itchy, blistering patches)
- Joint pain or stiffness without another explanation
- Mood changes — anxiety, irritability, or depression
- Unintentional weight loss or difficulty gaining weight
- Iron deficiency anemia that doesn’t respond to supplements
The digestive symptoms — bloating, gas, diarrhea, constipation, and abdominal pain — are the ones most people associate with gluten problems. But the “silent” symptoms often cause more long-term harm because they go unrecognized. Chronic fatigue, nutrient deficiencies (particularly iron, calcium, vitamin D, and B12), and neurological symptoms like peripheral neuropathy can all stem from gut damage that’s been present for years.
If you’re experiencing three or more of these symptoms consistently, it’s worth having a conversation with your healthcare provider about testing for celiac disease. The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) recommends starting with a tTG-IgA blood test — a simple, widely available screening tool.
The Science of Gluten and Gut Inflammation
When gliadin fragments cross the intestinal barrier, your immune system responds with inflammation — and that inflammatory response is at the root of nearly every symptom associated with gluten sensitivity and celiac disease.
Your body uses two branches of its immune system to respond to gluten. The innate immune response is fast and nonspecific — it treats gliadin as a general threat and triggers immediate inflammation. This is the response active in both celiac disease and non-celiac gluten sensitivity. The adaptive immune response, which is specific to celiac disease, produces targeted antibodies that attack the intestinal tissue itself. This is what makes celiac an autoimmune condition rather than just a sensitivity.
The inflammation doesn’t stay in your gut. Research from Dr. Fasano’s team and studies published in the Journal of Clinical Gastroenterology have shown that chronic intestinal inflammation can become systemic — spreading through the bloodstream to affect joints (inflammatory arthritis), skin (dermatitis herpetiformis), the brain (neurological symptoms, depression, anxiety), and the liver. This is why so many people with undiagnosed celiac disease present with symptoms that seem to have nothing to do with digestion.
Stress amplifies the whole cycle. When you’re under chronic stress, your body produces cortisol, which can further weaken tight junction integrity and suppress gut repair. The gut-brain axis — the communication highway between your digestive system and your central nervous system — means that gut inflammation can worsen anxiety, and anxiety can worsen gut inflammation. It’s a feedback loop that many GF families know all too well.
The good news: removing the trigger (gluten) interrupts this entire cascade. Studies indicate that most people with celiac disease show measurable improvement in intestinal inflammation within weeks of starting a strict gluten-free diet, with significant mucosal healing within 6–12 months.
How to Heal Your Gut After Gluten Exposure
Healing your gut is a process, not a one-time event. Whether you’ve just been diagnosed with celiac disease, identified a gluten sensitivity, or experienced accidental cross-contamination, these five steps provide a clear, science-backed framework for recovery.
- Remove the trigger completely. A strict gluten-free diet means eliminating all wheat, barley, rye, and their derivatives. This includes hidden sources like malt flavoring, soy sauce (unless tamari), and many processed foods. Even trace amounts — as little as 10 milligrams per day — can sustain intestinal damage in people with celiac disease. Read every label, every time.
- Support your body’s healing systems. Your gut lining regenerates every 3–5 days, but it needs resources to do so. Prioritize sleep (7–9 hours), manage stress through whatever works for you (walks, deep breathing, prayer, therapy), and stay hydrated. Your body does its most significant repair work during rest.
- Rebuild with targeted nutrition. Focus on whole, nutrient-dense foods that support gut lining repair: bone broth (rich in collagen and glutamine), leafy greens, wild-caught fatty fish, sweet potatoes, and ginger. Avoid ultra-processed GF substitutes during the active healing phase — they’re fine long-term, but whole foods give your gut more to work with early on.
- Restore your gut flora. A damaged gut often has a disrupted microbiome. Introduce probiotic-rich fermented foods gradually — plain yogurt (if tolerated), sauerkraut, kimchi, and kombucha. Consider a high-quality probiotic supplement with multiple strains. Start slowly to avoid digestive discomfort as your microbiome rebalances.
- Maintain with daily habits. Once you’re past the acute healing phase, prevention becomes the priority. Build sustainable habits: meal prepping to avoid last-minute unsafe food choices, keeping GF emergency snacks available, and establishing a daily routine that supports ongoing gut health.
How long does healing take? It varies significantly. Some people feel dramatically better within 2–4 weeks of going strictly GF. Complete mucosal healing in celiac disease typically takes 6–12 months in adults, though some studies suggest it can take up to 2 years. Children generally heal faster.
Best Foods for Gut Healing on a Gluten-Free Diet
What you eat after removing gluten matters just as much as removing gluten itself. These foods provide the specific nutrients your gut lining needs to repair, reduce inflammation, and restore a healthy microbiome.
Beyond these top six, also consider: bananas (especially slightly green — they contain prebiotic resistant starch), coconut oil (contains lauric acid with antimicrobial properties), collagen peptides (mix into smoothies or coffee for gut-lining support), aloe vera juice (soothes intestinal inflammation), and plain yogurt (if dairy is tolerated — provides both probiotics and protein).
A few foods to limit during active gut healing: alcohol, caffeine in large amounts, ultra-processed foods (even GF ones), artificial sweeteners, and high-sugar foods. These can slow healing by irritating an already compromised gut lining or disrupting your microbiome balance.
Supplements That Support Gluten and Gut Health Recovery
Supplements can accelerate gut healing — but they work best as part of a comprehensive approach that includes diet, stress management, and a strict GF lifestyle. They are not a shortcut, and they absolutely cannot replace removing gluten. Think of them as support, not a solution.
- Probiotics — Strain diversity matters more than mega-doses. Look for supplements with Lactobacillus and Bifidobacterium strains that are certified gluten-free. Research suggests multi-strain formulas support broader microbiome recovery after intestinal damage.
- L-Glutamine — This amino acid is the primary fuel for the epithelial cells that line your small intestine. Studies indicate that L-glutamine supplementation may support intestinal barrier repair, particularly during active healing. Typical doses range from 5–10 grams daily.
- Digestive Enzymes (DPP-IV) — Dipeptidyl peptidase IV enzymes help break down trace amounts of gluten from accidental cross-contamination. They are not a replacement for a GF diet and will not protect against intentional gluten consumption. Think of them as backup, not permission.
- Collagen Peptides — Emerging evidence suggests collagen supplementation may support gut lining integrity by providing the amino acids (glycine, proline, hydroxyproline) needed for tissue repair. Easy to add to smoothies, coffee, or soups.
- Zinc Carnosine — This compound has been studied for its ability to support mucosal integrity in the GI tract. Research published in the journal Gut found it can help stabilize the gut lining and reduce inflammation markers.
- Prebiotics — Prebiotic fibers (like inulin and fructooligosaccharides) feed the beneficial bacteria already in your gut. They’re the “fertilizer” to probiotics’ “seeds.” Introduce gradually to avoid gas and bloating.
Gut Health for Your Whole Family
If you’re managing a gluten-free household with kids, their gut health matters just as much as yours — arguably more. Children’s microbiomes are still developing, and early gut health patterns can influence immune function, allergy risk, and overall health for years to come.
Age-appropriate strategies make a big difference. For younger kids, focus on making gut-friendly foods fun and familiar — smoothies with collagen powder, “rainbow plates” with colorful vegetables, and yogurt parfaits with berries. For older kids and teens, involve them in meal prep and help them understand why these foods matter without making it feel like a restriction.
As a homeschooling mom of two boys, I can tell you that the family approach is everything. We don’t have separate “GF meals” — everyone eats the same food. That removes the stigma, reduces cross-contamination risk, and honestly just makes life simpler. Our boys know how to read labels, they know which restaurants we trust, and they understand that taking care of their gut is just part of how our family does things.
Building gut-healthy habits as a family — cooking together, choosing fermented foods at the store, talking openly about how different foods make us feel — creates a foundation that lasts well beyond childhood.
Frequently Asked Questions About Gluten and Gut Health
Can gluten damage your gut even if you don’t have celiac disease?
Yes. Research led by Dr. Alessio Fasano shows that gluten triggers zonulin release in many people, not just those with celiac disease. Non-celiac gluten sensitivity can cause intestinal inflammation, increased permeability, and real symptoms — even without the autoimmune antibodies or villous atrophy seen in celiac disease.
How long does it take for your gut to heal after going gluten-free?
Most people feel symptom improvement within 2–4 weeks of strict gluten elimination. Complete mucosal healing in celiac disease typically takes 6–12 months in adults, though some studies suggest up to 2 years for full recovery. Children generally heal faster, often within 3–6 months.
What does gluten do to your intestinal lining?
Gluten fragments trigger zonulin release, which opens the tight junctions between intestinal epithelial cells. This increases intestinal permeability, allowing bacteria and food particles into the bloodstream. In celiac disease, the immune response also destroys villi — the finger-like projections that absorb nutrients.
What are the first signs of gut damage from gluten?
Common early signs include persistent bloating after meals, irregular bowel habits (diarrhea, constipation, or both), unexplained fatigue, and brain fog. Less obvious signs include iron-deficiency anemia that doesn’t respond to supplements, skin rashes, joint pain, and mood changes like increased anxiety.
Do probiotics help with gluten sensitivity?
Research suggests probiotics can support gut recovery by restoring beneficial bacteria disrupted by gluten-related inflammation. Multi-strain formulas with Lactobacillus and Bifidobacterium species show the most promise. Probiotics do not treat celiac disease or replace a gluten-free diet, but they may reduce symptoms and support healing.
Can you reverse gut damage from gluten?
In most cases, yes. The intestinal lining regenerates every 3–5 days, and with strict gluten avoidance plus nutritional support, significant healing occurs within months. Studies show that the majority of celiac patients achieve substantial mucosal recovery within 1–2 years on a strict gluten-free diet.
Is leaky gut from gluten real?
Yes. Increased intestinal permeability (the clinical term for “leaky gut”) is a well-documented phenomenon in celiac disease and gluten sensitivity. Dr. Fasano’s research at Massachusetts General Hospital identified the zonulin pathway as the mechanism by which gluten increases permeability in susceptible individuals.
What supplements help repair the gut lining?
The most evidence-backed supplements for gut lining repair include L-glutamine (primary fuel for intestinal cells), zinc carnosine (supports mucosal integrity), collagen peptides (provides amino acids for tissue repair), and probiotics (restore beneficial gut bacteria). Always consult your healthcare provider before starting supplements.
Explore the Full Gut Health Guide
This page is the hub for our complete 25-article gut health resource library. Each guide dives deep into one specific topic so you get the detailed, actionable information you need. Click any title below to explore.
The Bottom Line
The relationship between gluten and gut health is real, well-researched, and — here’s the part I want you to hold onto — absolutely something you can manage. Whether you’re newly diagnosed with celiac disease, navigating non-celiac gluten sensitivity, or supporting a family member through the transition, the path forward is clear: remove the trigger, nourish your body with gut-healing foods, support recovery with targeted strategies, and build sustainable daily habits.
As a nurse and a mom living this lifestyle every day, I know it feels overwhelming at first. The label-reading, the meal planning, the questions from well-meaning family members who don’t quite get it — it’s a lot. But your gut is remarkably resilient. Give it the right conditions, and it will heal. You’ve already taken the most important step by learning about what’s happening in your body and why. Now you have the knowledge to take action.
Download our free 7-Day Gut Healing Meal Plan — a week of simple, delicious gluten-free meals designed to support your digestive health. Each day includes breakfast, lunch, dinner, and a gut-healing snack, with a complete grocery list so you can start this week.
This content is for educational purposes only and does not constitute medical advice. Always consult your healthcare provider for diagnosis, treatment decisions, and personalized guidance about your gut health and gluten-related conditions.
