No, people with celiac disease cannot safely reintroduce gluten — not even after years of feeling well on a gluten-free diet. If you have non-celiac gluten sensitivity (NCGS), the answer is more nuanced, but reintroduction still carries real risks and should never be done without medical guidance.
I hear this question all the time, especially from people who have been gluten-free for a while and start feeling great. “Maybe I don’t really need to be this strict anymore.” I get it. When my own diagnosis sank in, part of me held onto the hope that it was temporary. It’s a completely human response to a hard situation.
But the science here is pretty clear, and as a nurse and someone living this every day, I want to give you the honest, medically grounded answer — not false hope.
In this article, we’ll cover what actually happens to your gut when you reintroduce gluten, why “feeling fine” doesn’t mean you’re healed, the difference between celiac disease and non-celiac gluten sensitivity when it comes to reintroduction, and what the research actually says about tolerance developing over time.
Key Takeaways
- People with celiac disease cannot develop tolerance to gluten — the autoimmune response remains, even without obvious symptoms.
- Feeling better on a gluten-free diet does not mean celiac disease is “cured” or in remission in a way that allows gluten reintroduction.
- Non-celiac gluten sensitivity may allow for some dietary flexibility, but reintroduction should always be supervised by a gastroenterologist.
- Silent celiac disease — no symptoms but ongoing gut damage — is a real and serious risk for anyone with celiac who eats gluten.
- There are no FDA-approved treatments that currently allow safe gluten reintroduction for people with celiac disease.
Why Celiac Disease Does Not Go Into “Remission” With Reintroduction
Celiac disease is a lifelong autoimmune condition. When someone with celiac disease eats gluten, their immune system attacks the lining of the small intestine — specifically the villi, the tiny finger-like projections that absorb nutrients. This isn’t a food allergy that can be outgrown or a sensitivity that fades with time.
The key word here is autoimmune. According to the Celiac Disease Foundation, there is currently no cure for celiac disease, and the only effective treatment is strict, lifelong adherence to a gluten-free diet. The immune system’s memory of gluten as a threat does not reset, even after extended periods of avoidance.
Think of it this way: someone with a peanut allergy doesn’t lose their allergy after avoiding peanuts for two years. The same principle applies here, though the mechanism is different. Your immune system has learned to react to gluten, and that learning doesn’t unlearn itself.
The “I Feel Fine” Problem: Silent Celiac Disease
One of the most dangerous misconceptions in the gluten-free world is that symptom relief equals healing. Many people with celiac disease feel dramatically better within weeks or months of going gluten-free. That’s real, and it’s wonderful. But here’s what often happens next: they feel so good that they wonder if they ever really had a problem.
The truth is that intestinal healing takes significantly longer than symptom resolution. Research published in journals reviewed by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) suggests that complete intestinal healing in adults with celiac disease can take anywhere from one to several years — and some adults never fully heal even on a strict gluten-free diet.
Even more concerning is what’s called silent celiac disease — a pattern where gluten consumption continues to damage the intestinal lining, but the person experiences few or no noticeable symptoms. Someone with silent celiac disease might eat a piece of bread and feel completely fine, while their gut absorbs the hit invisibly.
This is why follow-up care with a gastroenterologist matters so much. Repeat antibody testing and sometimes repeat endoscopy are the only reliable ways to assess what’s actually happening in your small intestine — not how you feel day-to-day.
Non-Celiac Gluten Sensitivity: Is Reintroduction Ever Possible?
Non-celiac gluten sensitivity (NCGS) is a different condition — one that research is still actively working to understand. Unlike celiac disease, NCGS does not involve the same autoimmune intestinal damage, and people with NCGS do not test positive for the antibodies associated with celiac disease.
Because NCGS is not autoimmune in the same way, some researchers believe that certain individuals may be able to tolerate gluten reintroduction — at least in limited amounts — especially if the underlying triggers for their sensitivity change over time. However, this is not well-established, and the mechanisms behind NCGS are still debated in the medical community.
It’s also worth knowing that some people initially diagnosed with NCGS turn out to actually have celiac disease that was missed, or develop celiac disease later. This is exactly why any conversation about reintroduction needs to start with a clear, confirmed diagnosis — not an assumption.
If you have NCGS and want to explore whether you can reintroduce gluten, that conversation belongs with a gastroenterologist — ideally after updated testing to confirm you don’t have celiac disease. A supervised elimination and reintroduction protocol (similar to what’s used in a low-FODMAP diet approach) may be appropriate for some people with NCGS, but this is not something to do on your own.
What Actually Happens When Someone With Celiac Reintroduces Gluten
Let’s talk about what happens at the biological level, because I think understanding the mechanism helps make the “why” clearer.
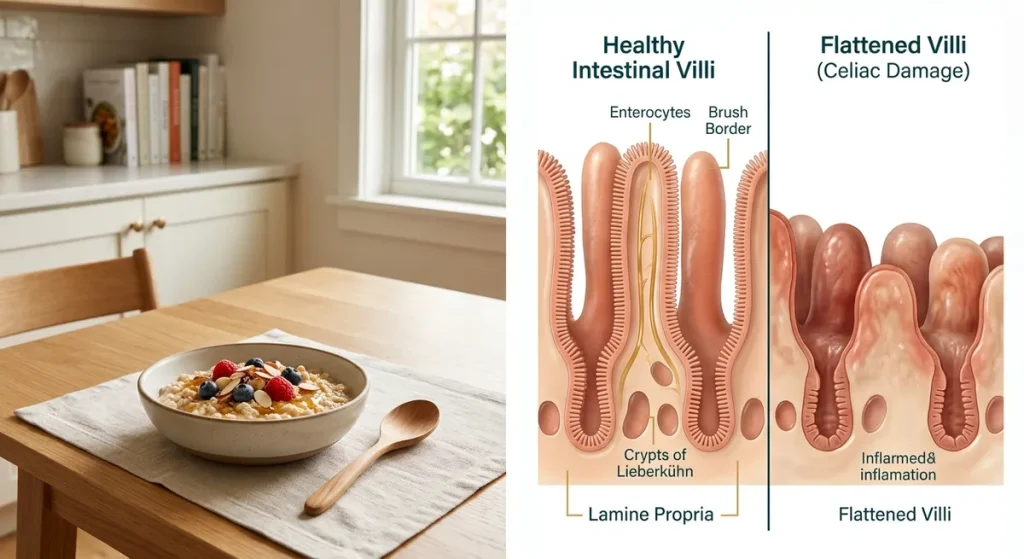
When someone with celiac disease eats gluten, the protein (specifically gliadin, a component of gluten) triggers an immune response. The body produces antibodies — including tissue transglutaminase IgA (tTG-IgA) — and the immune system attacks the intestinal villi as collateral damage. Over time, this causes villous atrophy: the villi flatten and shrink, dramatically reducing the surface area available to absorb nutrients.
The cumulative damage from repeated gluten exposure — even occasional or accidental — can lead to serious long-term complications. The Beyond Celiac organization notes that untreated or poorly managed celiac disease is associated with increased risk of lymphoma, ongoing malnutrition, and neurological complications.
If you’ve ever had an accidental gluten exposure and felt awful, you already have a window into this process. And if you’ve had accidental exposures and felt fine — that’s the silent damage scenario, and it’s arguably more concerning.
What About Emerging Research and Future Treatments?
Here’s the hopeful part — and I genuinely mean that. There is active, meaningful research happening right now aimed at finding treatments that might one day allow people with celiac disease to tolerate some gluten exposure.
Approaches being studied include enzyme therapies that could break down gluten before it triggers an immune response, immune-modulating drugs, and oral tolerance induction protocols. As of now, none of these have received FDA approval for use in celiac disease, and none should be interpreted as a green light to start eating gluten today.
The Mayo Clinic confirms that the current standard of care for celiac disease remains a strict, lifelong gluten-free diet — full stop. Staying informed about research is smart. But “there might be a treatment someday” is not the same as “it’s safe to try gluten now.”
Common Mistakes to Watch Out For
Mistakes People Make When Thinking About Reintroducing Gluten
- Assuming symptom relief means the disease is gone — symptoms and gut health are not the same thing.
- Testing gluten reintroduction without medical supervision or updated diagnostic testing.
- Confusing celiac disease with NCGS when deciding whether reintroduction is safe.
- Believing that “a little bit” of gluten is okay because you don’t feel it — silent damage is real.
- Relying on at-home food sensitivity tests instead of proper celiac antibody bloodwork and endoscopy.
- Stopping a gluten-free diet before consulting a gastroenterologist about a dietary gluten challenge for retesting purposes.
Frequently Asked Questions
No — not if you have celiac disease. Feeling healed and being healed at the intestinal level are two different things. Celiac disease is a lifelong autoimmune condition, and the immune response to gluten remains even after extended periods of avoidance. Reintroduction will restart the immune attack on your intestinal lining, whether or not you feel symptoms.
If you’re considering a gluten challenge to confirm a celiac diagnosis (for example, if you went GF before proper testing), the current standard recommendation from gastroenterologists is to consume a meaningful amount of gluten — typically 1-2 slices of regular wheat bread per day — for at least 2-6 weeks before repeat antibody testing or endoscopy. This must be done under medical supervision. Never do this on your own.
It’s possible — but this question should be answered by a gastroenterologist with proper testing, not by experimenting with gluten at home. If you have doubts about your original diagnosis, ask your doctor about a supervised gluten challenge followed by repeat endoscopy. Don’t self-diagnose your way out of a medical condition.
No. Celiac disease is not outgrown. It is a lifelong autoimmune condition regardless of when it develops. Children diagnosed with celiac disease require a strict gluten-free diet for life. If your child’s symptoms have improved, that’s a sign the diet is working — not that the disease is gone. Always follow up with a pediatric gastroenterologist for ongoing monitoring.
If you have confirmed non-celiac gluten sensitivity (not celiac disease), some people do tolerate small amounts of gluten over time, especially if the root cause was something else like IBS or FODMAPs. However, any reintroduction should be guided by a gastroenterologist and preceded by updated testing to rule out celiac disease definitively. Don’t assume — confirm first.
The Honest Answer on Gluten Reintroduction
If you have celiac disease, you cannot safely reintroduce gluten — not after six months, not after six years, not ever. The autoimmune mechanism that causes intestinal damage does not switch off with avoidance. Feeling great on a gluten-free diet is a sign that the diet is doing its job, not a sign that the disease has resolved. Staying gluten-free is how you protect your gut, your nutrient absorption, and your long-term health.
If you have non-celiac gluten sensitivity and are wondering about dietary flexibility, that’s a more nuanced conversation — but still one that belongs with a gastroenterologist who knows your full history, not a self-experiment in your kitchen. Get tested, get clear answers, and then make decisions with your doctor’s input.
Living gluten-free for life is genuinely hard. It’s expensive, it’s socially exhausting, and there are days when the whole thing feels deeply unfair — because it is. But the research is consistent: for people with celiac disease, a strict gluten-free diet is the only evidence-based treatment we have. You deserve accurate information to make that commitment with clarity and confidence, not false hope.
